Positive Reviews



It is proven that a different model is needed in today’s margin-crunched world in order to profitably run a DME business. Our model is the right fit, immediately saving you money & getting more done for less directly adding to your profit margin.
Working remotely from our operations center, our team connects to your office via a secure internet connection to execute time consuming yet important tasks, like order entry, verifications to billing & denial management on your behalf. This allows our clients to utilize their best staff for more valuable tasks.
Advanced solutions for financial care built for healthcare clients. Patron’s satisfaction enriched dramatically by improving our compliance & reducing forfeits to create an efficient claims progression, the medical billing process at FutureBoxx follows a series of clearly defined steps with a complete focus on accuracy, quality and process audits from end to end.
Read MoreOne of the most important processes after care is rendered is to ensure that all data is captured completely and correctly so that a clean claim is produced for billing.
Our Order/ Charge Capture Solution creates flawless data entry of services that have been delivered to patients, including the inputting of all coded services, relevant modifiers, patient and payer information. Our Coding Solution includes selecting appropriate diagnosis codes, procedure codes and modifiers as well as following all applicable government and payer rules & regulations. Our educated and well-trained staff ensures that all of these variables are recognized without errors, and produce correctly coded invoices. Our continuous quality assurance program ensures that there are minimal keying errors, and we constantly update correct coding requirements from insurance companies.
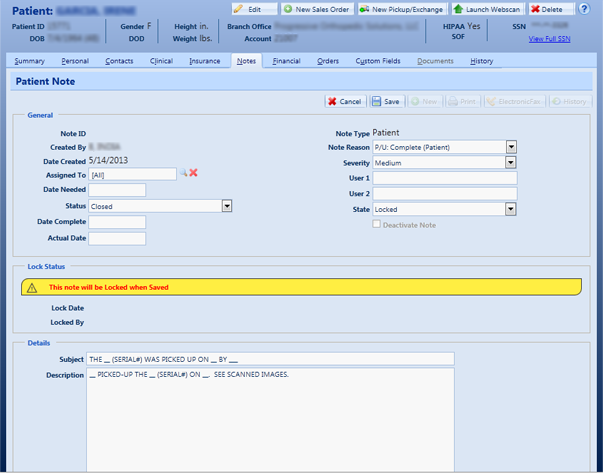

The Insurance Benefits Eligibility Verification Solution provides accurate, real-time validation of patients’ insurance and benefit coverage levels. This process is handled by a team of dedicated Eligibility Verification experts who work with the insurance provider to clearly identify the patients’ insurance coverage and financial obligations are valid and correct, and ensure the provider records match the patient information.
FutureBoxx medical billing team ensures that every new or continuing patient’s verification is completed prior to his or her arrival for the first appointment. This vital confirmation prior to the service being rendered helps ensure that the rules required by the payer are followed, that the patient understands his/her financial obligations as well as validating the payment to be expected either by the patient and/or the payer.
We offer comprehensive document retrieval services to Physicians and Providers of equipment and supplies that are medically necessary for billing or otherwise.
Physicians Order Retrieval
We offer a flat fee per document completed, with complete verification and reporting.
Medical Notes Retrieval
We will collect and verify medical notes for compliance with Medicare on High Frequency Testers. Forms are verified for specific information defined by our clients.


Our focus is on creating patron-hub & transformational operating simulations for Healthcare clients to better manage their connexion services. Our solutions upsurge quality, reduce dispatch time and drive efficiency. FutureBoxx provides clients with a structure for supervising the routine of healthcare resources & assessing the relevance of unified care.
As mentioned above, we’re a solution for all your business management including delivering the tickets, we do assist the healthcare provider as well, by fulfilling the medical billing solution which you can count on. Eases the administrative costs through dynamic processes & makeover initiatives.
Our Billing Solution helps providers provide clean, scrubbed, and error-free claims to the payers. This solution includes processing for electronic and paper claims, where our team of experts provision customized editing to help identify and rectify issues prior to the submission of claims, leading to submission of cleaner claims. This pre-submission scrubbing results in fewer denials, faster and accurate payments.
The solution also covers paper claims along with any and all payer required attachments. Our team maintains clear definitions of payer requirements, help our clients provide the right medical notes and records, and furnish the primary explanation of benefits for correct adjudication of claims.

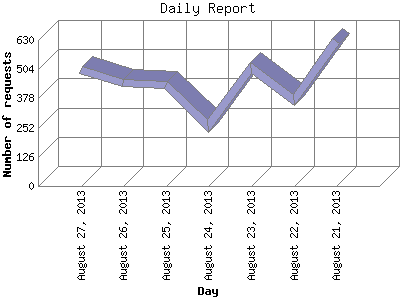
With our in-depth experience in Brightree, our team pulls out reports for management review as and when required. This not only helps clients make knowledgeable decisions it helps cash flow and overall efficiency of the business.
Medical records of patients at a hospital contain demographic details about the patient, summary of his/her medical history, summary of diagnoses and regular medical updates on each physician visit. It is implied that the hospital or healthcare facility receives the final payment only when the insuring agency settles the claim.
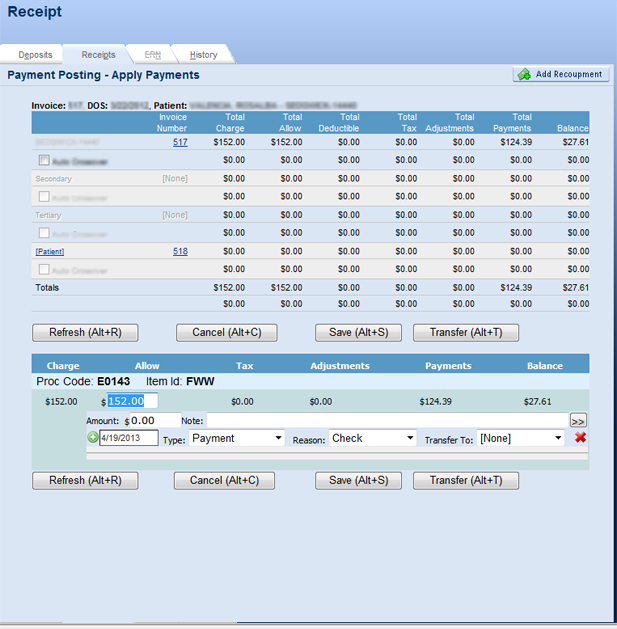
Health care service providers are constantly struggling between hiring teams to manage the business or to provision services. While the former is important, it is not core to the care provider business. Our team brings years of experience in Payment Posting Services that encompasses managing cash receipts, payment posting, and reconciliation.
Our team of highly skilled and analytical staff enables timely and accurate posting of payments, payer correspondence, and contractual adjustments. Additionally our services include reconciling EFT payments, lock box activity, and EOB scanning and retrieval. Shifting these tasks to the payment posting team results in a dedicated and trained work force that is solely focused on correct posting and account resolution.
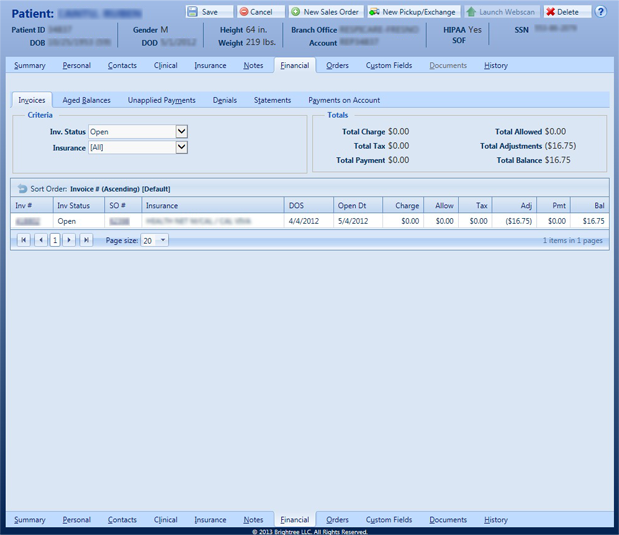
Are your claims in the limbo ? Don't Know the status of your pending claims with insurance carriers ? We can call on your behalf to find out the status of each claim so you can plan the next steps accordingly.
Advanced solutions for financial care built for healthcare clients. Patron’s satisfaction enriched dramatically by improving our compliance & reducing forfeits to create an efficient claims progression, the medical billing process at FutureBoxx follows a series of clearly defined steps with a complete focus on accuracy, quality and process audits from end to end.
Our Denial Management service helps clients navigate the complex and time-consuming claims denials from payers. Our skilled team provides deep analysis and insight into every denial a client receives. We then work on two strategies:
The Denial Management team works closely with the payer and provider to resolve these issues. We also will frequently re-engineer the processes internally and at the providers' offices, so we stay ahead of the denial process.
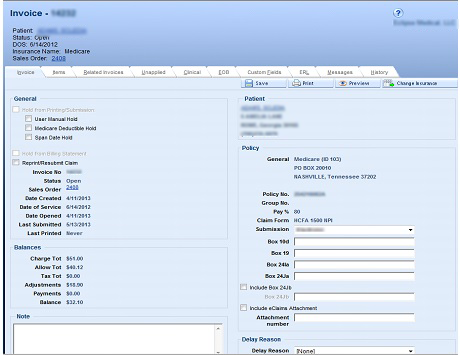
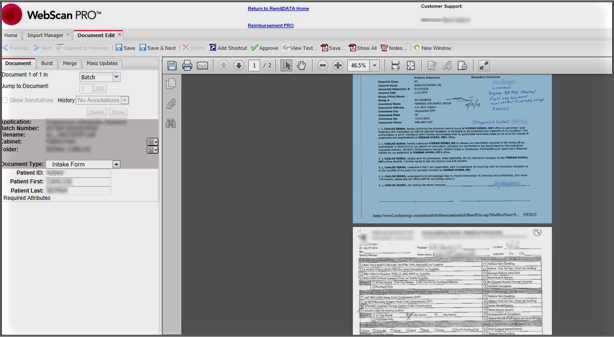
If your DME uses a document management system to attach patient records to the patient on brightree, we attach the same to the patient as needed giving you immediate compliance and access to patient records anytime.

More than 100,000 software applications
Positive Reviews
Awards Won
Top Tech Pros
Satisfied Customers
Start your free trial. No credit card required. No strings attached.
It also gives us enough time to understand your products & processes.
What Does It Cover:
Once you fill the form an account manager will be in touch with you within 2 business days to go over next steps.